Category: Articles
All the latest articles, blogs and stories from the world of inclusion health.
1st April 2022
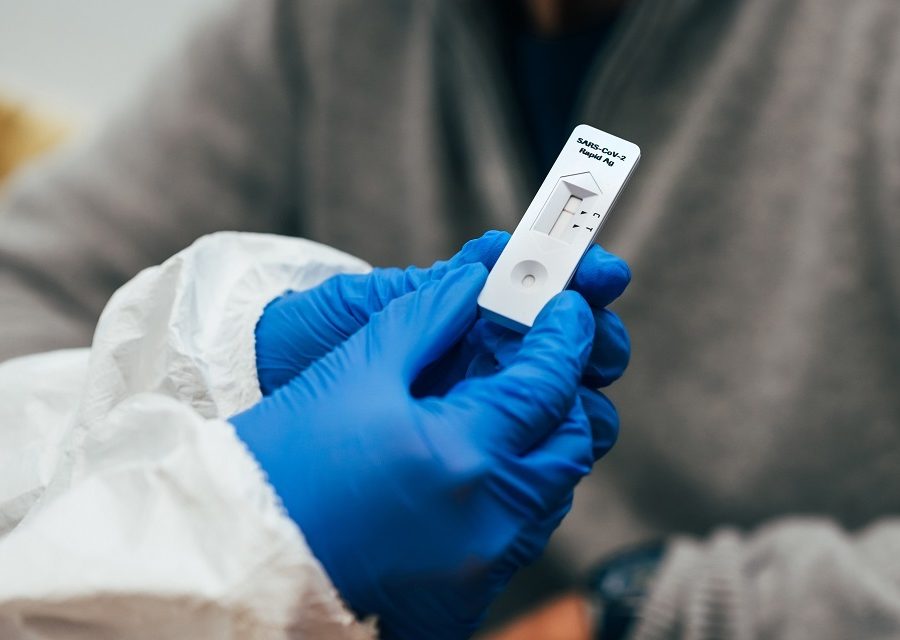
Free Covid-19 tests to continue for high-risk settings, including homelessness settings
Government responds to call for continued Covid-19 tests for homeless services.
11th January 2022
Pathway joins call for the Health and Care Bill to tackle extreme health inequalities
20th January 2021
New street outreach guidelines launched
15th October 2019
Homeless hospital discharge nursing
31st October 2017
'A Second Class Ending'
31st October 2017
Is Your Surgery 'Homeless Ready'?
4th July 2017
Homeless Patients Are Dying Without Support
18th November 2014
Well done Tim!
3rd October 2014
Brighton & Sussex University Hospital
3rd October 2014